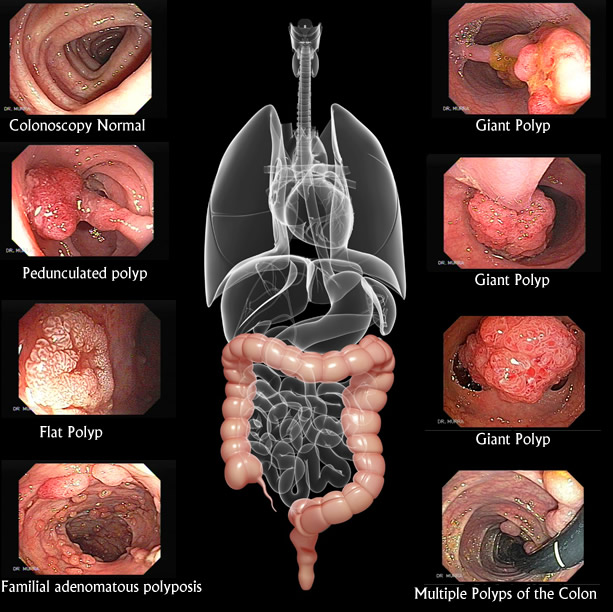
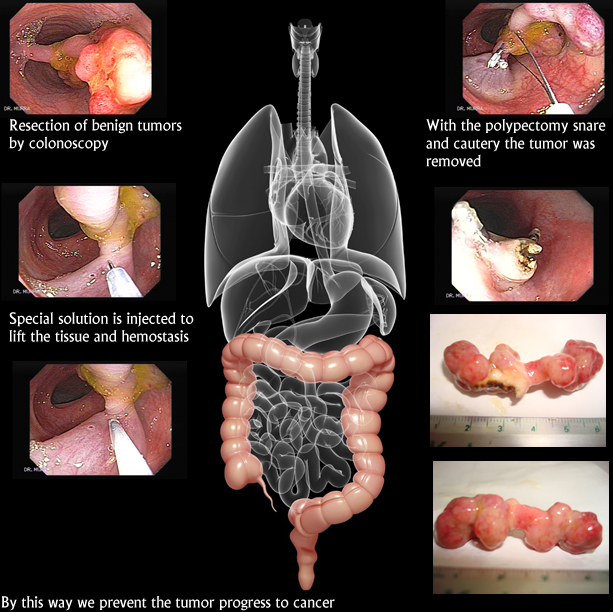
COLORECTAL CANCER
Colorectal Cancer (CRC) is a common, lethal, and preventable disease
CRC is the second leading cause of cancer death in both sexes, accounting for 10 to 11 percent of cancer deaths overall; it is third most common in men and women separately. Approximately one in three people who develop CRC die of this disease.
Colorectal Cancer is another frequent neoplasia in the republic of El Salvador representing the fourth most frequent Cancer according to national statistics, with its incidence on the rise. The clinical course of colon cancer is usually silent and initially without symptoms until the disease has reached an advanced stage. In order to find cancerous or pre-cancerous lesions at an early, curable stage a total video-colonoscopy is recommended at 5 year intervals, for any person 30 years and up. For patients with family history of colon cancer or colon polyps a yearly screening is advised. Unfortunately, most people do not follow these recommendations, putting themselves at risk of dying of colon cancer or living with bothersome cololostomy for the rest of their lives. One of the main purposes of the colonoscopy is the screenning for polyps. Polyps are small or medium sized tumors which grow without symptoms some of them may evolve into cancer.if these are detected early they can be removed endoscopicaly with a procedure call polypectomy.
Colorectal Cancer
Adenoma-carcinoma sequence — Most colorectal cancers arise from adenomatous polyps, some of which progress from small (<5 mm) to large polyps (>1.0 cm), and then to dysplasia and cancer. This progression probably takes at least 10 years in most people; the distribution of progression times is not precisely known because polyps are ordinarily removed when they are found. Neoplastic changes are accompanied by, and probably result from, an accumulation of genetic defects. Some cancers also apparently arise from adenomas that are not polypoid.Large flat adenomas were more likely to contain dysplastic changes than small ones, as is the case for polypoid adenomas. The true proportion and clinical significance of adenomas that are flat is uncertain.
Two-thirds of polyps are adenomas. The prevalence of adenomas is about 25 percent by age 50 and 50 percent by age 70. Large adenomatous polyps (>1 cm), the size most likely to progress to cancer, are less common (3 to 5 percent) than small adenomas.
The risk of CRC increases with polyp size, number, and histology (eg, villous worse than tubular architecture). The characteristics of an individual polyp are a marker for the colon as a whole; thus, the polyp examined is representative of the individual's propensity to form polyps and cancer.
A cancer is an uncontrolled proliferation of cells.
Is very common, usually occurring after the age of 50. The existence of polyps (protrusions of tissue from the wall of the bowel into the lumen) generally precedes the development of colorectal cancer. Polyps are painless but can bleed, causing blood to be present in the stool. The progression to cancer usually does not occur until after the age of 40 unless there is a genetic-linked familial disorder. Routine medical examination helps detect colorectal cancer at early stages, thereby improving the likelihood of successful treatment. Simple tests to chemically detect small amounts of blood in the stool that are not visible to the eye can be easily performed in the home.
Both polyps and colon cancer occur much more frequently in Western societies where the diets are low in fruits, vegetables, protein from vegetable sources and fiber. Smoking and drinking alcoholic beverages appear to increase the risk of polyp formation. Evidence suggests that diets high in calcium, folic acid and fiber act as chemopreventive agents, reducing the risk of colorectal cancer. There is evidence that use of some nonsteroidal anti-inflammatory drugs (NSAIDs) prevents polyp progression to cancer in certain people.
Determining risk — Before deciding how to screen, clinicians should decide whether the individual patient is at average or increased risk. A few simple questions are all that is necessary: Do you have a family history of colorectal cancer? If so, in first degree relatives, at what age of onset, and how many?
Have you had a personal history of colorectal cancer or adenomatous polyps?
Have you had inflammatory bowel disease?
The patient is considered average risk if the answer to all these questions is "no." Patients answering yes to any of these questions need to be evaluated further.
Colonoscopy: Colon Cancer Descending Colon
Colonoscopy of Colon Cancer
Frequently Asked Questions About Colorectal Cancer
1. I'm a 40 year-old man with no family history of colorectal cancer or polyps. Should I start getting tested for colon cancer? What are the different types of tests for this cancer?
Because you don't have a family history of colorectal cancer or polyps, you are considered at average risk for colorectal cancer. Men with average risk should begin prevention examinations at age 40. The recommended screening tests to detect early-stage lesions and polyps for men at average risk include:
- Fecal occult blood test This test examines the stool for blood not easily noticed by the naked eye. For men at average risk of colorectal cancer, this test should be performed every year starting at age 50.
- Flexible sigmoidoscopy Flexible sigmoidoscopy is a routine outpatient procedure in which a physician uses a sigmoidoscope (a long, flexible instrument about a 1/2-inch in diameter) to view the lining of the rectum and the lower third of the colon (called the sigmoid and descending colon). This test is usually done every 5 years and can be used in combination with the yearly fecal occult blood test.
- Air contrast barium enema Sometimes, a doctor will use a test called air contrast barium enema. This test is an X-ray examination of the entire colon and rectum in which barium and air are introduced gradually into the colon by a rectal tube to improve visualization. Doctors typically recommend this test (sometimes in combination with flexible sigmoidoscopy) every five years, starting at age 50.
- Colonoscopy This is an outpatient procedure in which the rectum and the inside of the entire colon are examined. During a colonoscopy, a doctor uses a long, flexible instrument about a 1/2-inch in diameter to view the lining of the colon. This test is recommended every 10 years, starting at age 50.
2. I found a little bit of blood in my stool. Could I have colorectal cancer?
The earliest sign of colorectal cancer may be bleeding. But if you find blood in your stool, don't panic. A number of different illnesses can cause bleeding, not just colon cancer. If you find blood in your stool, see your doctor so that a correct diagnosis can be made and proper treatment received.
Other symptoms to look out for if you suspect colon cancer include:
- Change in bowel habits (constipation or diarrhea)
- Unusual stomach or gas pains
- Very narrow stool
- A feeling that the bowel has not emptied completely after passing stool
- Unexplained weight loss
- Fatigue
Q. How do I prevent colon-rectal (colorectal) cancer?
A. Although colorectal cancer is one of the most common types of cancer in the United States, scientists are trying to learn more about what causes the disease and how it can be prevented.
Doctors do not yet know why one person gets colorectal cancer and another does not, but they do know that no one can catch colorectal cancer from another person. Cancer is not contagious.
People can lower their risk of getting colorectal cancer. For example, those who have colorectal polyps (nodular growths of tissue developing in the lining of a cavity, which may be benign or malignant), should talk with the doctor about having them removed. People can also change their eating habits to cut down on fat and increase the amount of fiber (roughage) in their diet.
Q. What are the risk factors for developing colorectal cancer?
A. Some people are more likely to develop colorectal cancer than others. Studies have found that certain factors increase a person’s risk. The following are risk factors for this disease:
- Polyps – Most (perhaps all) colorectal cancers develop in polyps. Polyps are benign, but they may become cancerous over time. Removing polyps is an important way to prevent colorectal cancer.
- Age – Colorectal cancers occur most often in people who are over the age of 50, and the risk increases as people get older.
- Family history – Close relatives of a person who has had colorectal cancer have a higher than average risk of developing the disease. The risk for colon cancer is even higher among members of a family in which many relatives have had it. (In such cases, the disease is called familial colon cancer.)
- Familial polyposis – This is an inherited condition in which hundreds of polyps develop in the colon and rectum. Over time, these polyps can become cancerous. Unless the condition is treated, a person who has familial polyposis is almost sure to develop colorectal cancer.
- Diet – The risk of developing colon cancer seems to be higher in people whose diet is high in fat, low in fruits and vegetables, and low in high-fiber foods such as whole-grain breads and cereals.
- Ulcerative colitis – This disease causes inflammation of the lining of the colon. The risk of colon cancer is much greater than average for people who have this disease, and the risk increases with the length of time they have had it.
Q. What can I do to detect it?
A. Most health problems respond best to treatment when they are diagnosed and treated as early as possible. This is especially true of colorectal cancer. Treatment is most effective before the disease spreads.
People can take an active role in the early detection of colorectal cancer by following these guidelines:
- During regular checkups, have a digital rectal exam. For this exam, the doctor inserts a lubricated, gloved finger into the rectum and feels for abnormal areas.
- Beginning at age 40, have an annual fecal occult blood test. This test is a check for hidden (occult) blood in the stool. The test is done because colorectal cancer may cause bleeding that cannot be seen. However, other conditions also may cause bleeding, so having blood in the stool does not necessarily mean a person has cancer.
- Beginning at age 50, have a sigmoidoscopy/colonoscopy every 3 to 5 years. (Speak with your doctor.) This is an exam of the rectum and lower colon using a sigmoidoscope. The doctor looks through a thin, lighted tube to check for polyps, tumors or other abnormalities.
- People who may be at a greater than average risk for colon cancer should discuss a schedule for these or other tests with their doctor.
Q. What are the symptoms of colorectal cancer?
A. Colorectal cancer can cause many symptoms. Warning signs to watch for include:
- Change in bowel habits
- Diarrhea or constipation
- Blood in or on the stool (either bright red or very dark in color)
- Stools that are narrower than usual
- General stomach discomfort (bloating, fullness and/or cramps)
- Frequent gas pains
- A feeling that the bowel does not empty completely
- Weight loss with no known reason
- Constant tiredness
These symptoms also can be caused by other problems such as ulcers, an inflamed colon or hemorrhoids. Only a doctor can determine the cause.
People who have any of these symptoms should see their doctor. The doctor may refer them to a doctor who specializes in diagnosing and treating digestive problems (a gastroenterologist).
Q. How will I be diagnosed for colorectal cancer?
A To find the cause of symptoms, the doctor will ask about your personal and family medical history. He will do a physical exam, and may order laboratory tests. In addition to the exams discussed above, the doctor may also order the following tests:
- Lower GI series – X-rays of the colon and rectum (the lower gastrointestinal tract). The x-rays are taken after the patient is given an enema with a white, chalky solution containing barium. (This test is sometimes called a barium enema.) The barium outlines the colon and rectum on the x-rays, helping the doctor find tumors or other abnormal areas. To make small tumors easier to see, the doctor may expand the colon by carefully pumping in air during the test. This is called an air contrast or double-contrast barium enema.
- Colonoscopy – An examination of the inside of the entire colon using a colonoscope, an instrument similar to a flexible sigmoidoscope, but longer.
If a polyp or other abnormal growth is found, the doctor can remove part or all of it through a sigmoidoscope or colonoscope. A pathologist examines the tissue under a microscope to check for cancer cells. This procedure is called a biopsy. Most polyps are benign, but a biopsy is the only way to know for sure.
If the pathologist finds cancer, the patient’s doctor needs to learn the stage, or extent of the disease. Staging exams and tests help the doctor find out whether the cancer has spread and, if so, what parts of the body are affected. Treatment decisions depend on these findings.
Staging may include x-rays, ultrasonography or CT (or CAT) scans of the lungs and liver, because colorectal cancer tends to spread to these organs. The doctor may order blood tests to measure how well the liver is functioning. The doctor also may do a blood test called a CEA assay. This test measures the blood level of carcinoembryonic antigen (CEA), a substance that is sometimes found in higher-than-normal amounts in people who have colorectal cancer, especially when the disease has spread.
Q. What do I need to know about the treatment for colorectal cancer?
A. The doctor develops a treatment plan to fit each patient’s needs. Treatment for colorectal cancer depends on the size and location of the tumor, the stage of the disease, the patient’s general health, and other factors.
Most people who have cancer want to learn all they can about the disease and their treatment choices so they can take an active part in decisions about their medical care. It helps to make a list of questions before seeing the doctor. Here are some questions you may want to ask before treatment begins:
- What is the stage of the disease?
- What are my treatment choices? Which do you suggest for me? Why?
- Would a clinical trial be appropriate for me?
- What are the expected benefits of each treatment?
- What are the risks and possible side effects of each treatment?
- What can be done about side effects?
- What can I do to take care of myself during therapy?
- What is the treatment likely to cost?
Patients and their loved ones are naturally concerned about the effectiveness of the treatment. Sometimes they use statistics to try to figure out whether the patient will be cured, or how long her or she will live. It is important to remember, however, that statistics are averages based on large numbers of patients. They cannot be used to predict what will happen to a particular person because no two cancer patients are alike.
People should feel free to ask the doctor about the chance of recovery (prognosis), but even the doctor does not know for sure what will happen. When doctors talk about surviving cancer, they may use the term remission rather than cure. Even though many patients recover completely, doctors use this term because the disease can come back.
Q. What about a second opinion?
A. Treatment decisions are complex. Sometimes it is helpful for patients to have a second opinion about the diagnosis and the treatment plan. Some insurance companies require a second opinion; others provide coverage for a second opinion at the patient’s request. There are several ways to find another doctor to consult:
- Your doctor may be able to suggest a doctor who specializes in treating colorectal cancer. Specialists who treat this disease include surgeons, medical oncologists, gastroenterologists and radiation oncologists.
- Patients can get the names of doctors from their local medical society, a nearby hospital or a medical school.
- Cancer information lines can tell callers about treatment facilities, including cancer centers and other National Cancer Institute-supported programs.
Q. What methods of treatment are available for colorectal cancer?
A. Colorectal cancer is generally treated with surgery, chemotherapy and/or radiation therapy. New treatment approaches such as biological therapy and improved ways of using current methods are being studied in clinical trials. A patient may have one form of treatment or a combination.
Surgery is the most common treatment for colorectal cancer and may be the only treatment needed. The type of operation depends on the location and size of the tumor. Most patients have a partial colectomy. In this operation, the surgeon takes out the part of the colon or rectum that contains the cancer and a small amount of surrounding healthy tissue.
Usually, lymph nodes near the tumor are removed during surgery to help the doctor be more accurate about the stage of the cancer.
In most cases, the surgeon reconnects the healthy sections of the colon or rectum. This part of the surgery is called anastomosis. If the healthy sections of the colon or rectum cannot be reconnected, the doctor performs a colostomy, creating an opening (stoma) in the abdomen through which solid waste leaves the body. The patient uses a special bag to cover the stoma and collect waste. A colostomy may be temporary or permanent.
A temporary colostomy is sometimes needed to allow the lower colon or the rectum to heal after surgery. Later in a second operation, the surgeon reconnects the healthy sections of the colon or rectum and closes the colostomy. The patient’s bowel functions soon return to normal.
Although it may take some time to adjust to a colostomy, most patients return to their normal lifestyle. A nurse or an enterostomal therapist teaches the patient how to care for a colostomy.
Chemotherapy is the use of drugs to kill cancer cells. Chemotherapy is sometimes given after surgery for colorectal cancer to try to prevent the disease from recurring, or coming back. This additional treatment is called adjuvant therapy. The doctor may use one drug or a combination of drugs.
Chemotherapy and radiation therapy are sometimes given to shrink the tumor prior to surgery.
Chemotherapy is usually given in cycles: a treatment period followed by a recovery period, then another treatment period, and so on. Anticancer drugs may be taken by mouth or given by injection into a blood vessel or body cavity. Chemotherapy is a systemic therapy, meaning that the drugs enter the bloodstream and travel through the body.
Here are some questions you may want to ask about chemotherapy:
- What is the goal of this treatment?
- What drugs will I be taking? What will they do?
- Will the drugs cause side effects? What can I do about them?
- How long will I need to take this treatment?
Researchers are studying ways of putting chemotherapy drugs directly into the area to be treated. For colorectal cancer that has spread to the liver, drugs can be injected into a blood vessel that leads directly to the liver. (This treatment is called intrahepatic chemotherapy.) Researchers are also investigating a method in which the doctor puts anticancer drugs directly into the abdomen during or after surgery. (This is called intraperitoneal chemotherapy.)
Usually a person has chemotherapy as an outpatient at the hospital, at the doctor’s office or at home. However, depending on which drugs are given, how they are given, and the patient’s general health, a short hospital stay may be necessary.
Radiation therapy (also called radiotherapy) is the use of high-energy rays to damage cancer cells and stop them from growing. Like surgery, radiation therapy is local therapy; it can affect cancer only in the treated area. Radiation is sometimes used before surgery to shrink a tumor so that it is easier to remove. More often, radiation therapy is given after surgery to destroy any cancer cells that may remain in the area. It may also be given to relieve pain or other problems in patients whose tumors cannot be surgically removed. Radiation therapy is usually given on an outpatient basis in a hospital or clinic five days a week for several weeks.
Researchers are conducting clinical trials to look for more effective ways of using radiation therapy. For example, some are studying the benefits of using radiation both before and after surgery ("sandwich" technique), and others are giving radiation during surgery (intraoperative radiation). Doctors are also exploring the use of radiation therapy alone (instead of surgery) for rectal cancer that has not spread.
Here are some questions you may want to ask your doctor before receiving radiation therapy:
- How will the radiation be given?
- What is the goal of this treatment?
- When will the treatment begin? When will it end?
- What can I do to take care of myself during treatment?
Biological therapy is a cancer treatment that helps the body’s immune (defense) system attack and destroy cancer cells. For some patients, biological therapy may be combined with chemotherapy as adjuvant treatment after surgery. Patients may need to stay in the hospital while receiving some types of biological therapy.
Q. What should I know before surgery?
A. These are some questions you may want to ask the doctor before surgery:
- What kind of operation will it be?
- How will I feel afterward? If I have pain, how will you help me?
- Will I need a colostomy? Will it be temporary or permanent?
- How long will I be in the hospital?
- Will I have to be on a special diet? Who will teach me about my diet?
- When can I return to my regular activities?
- Will I need additional treatment?
Q. What are the side effects of treatment?
A. It is often hard to limit the effects of therapy so that only cancer cells are removed or destroyed. Because healthy tissue may also be damaged, treatment can cause unpleasant side effects.
The side effects of cancer treatment are different for each person, and they may even be different from one treatment to the next. Doctors try to plan treatment in ways that keep side effects to a minimum, and they can help with any problems that occur. For this reason, it is very important to let the doctor know about any health problems during or after treatment.
Note: Regular follow-up exams are very important after treatment for colorectal cancer. The cancer can recur at or near the site of the original tumor or can spread to another area of the body. The doctor will continue to check closely so that, if the cancer comes back, it can be treated again as soon as possible.
Often, a social worker or enterostomal therapist at the hospital or clinic can suggest groups that can help with rehabilitation, emotional support, financial aid, transportation or home care.
Endoscopy of Colon Cancer, of the Cecum
These images are obtained by the video colonoscopy.
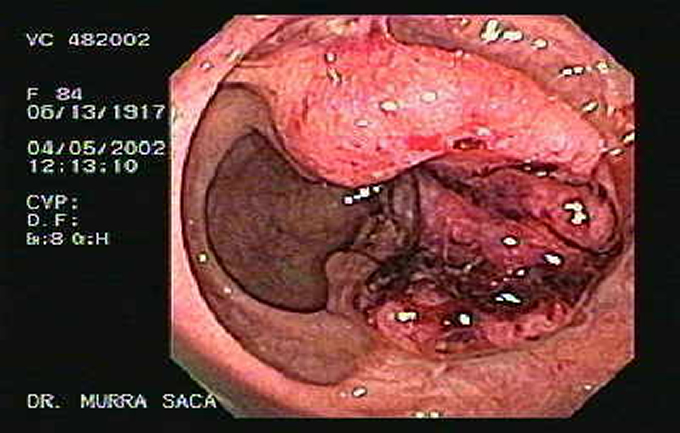
Endoscopic Image of Colorectal Cancer
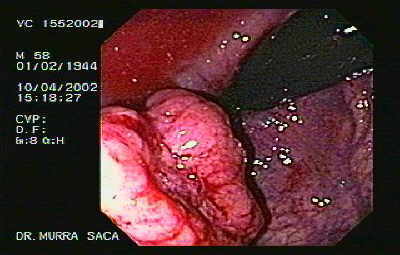
Rectal Cancer
Retroflexion image, we see the black part colonoscope
which is bent the end to make the move to look back.
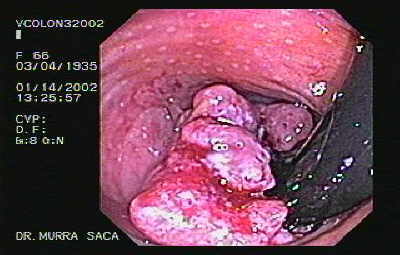
Rectal Cancer retroflexion image.
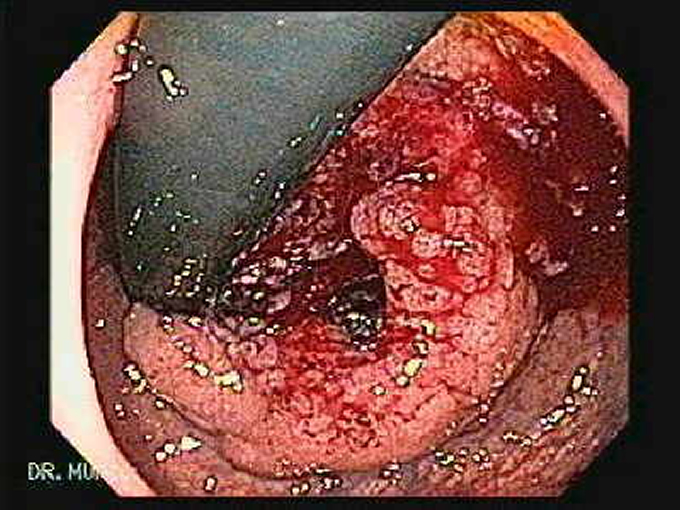
Rectal Cancer retroflexion image.
The Colorectal Cancer is another common cancer in El Salvador is fourth in the statistics, the incidence is increasing as more frequent and detect its evolution is usually silent causing no symptoms until it is in advanced stage , recently in El Salvador are seeing an increase colon cancer in young people, this phenomenon makes us reflect on the prevention of this cancer.
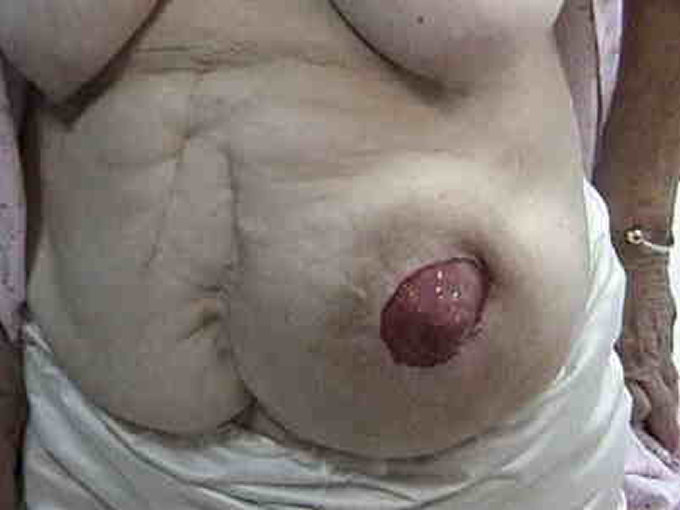
Colostomy: Female patient suffered from rectal bleeding and for two years was self
prescribed suppositories and ointments for hemorrhoids alleged, was found rectal cancer.
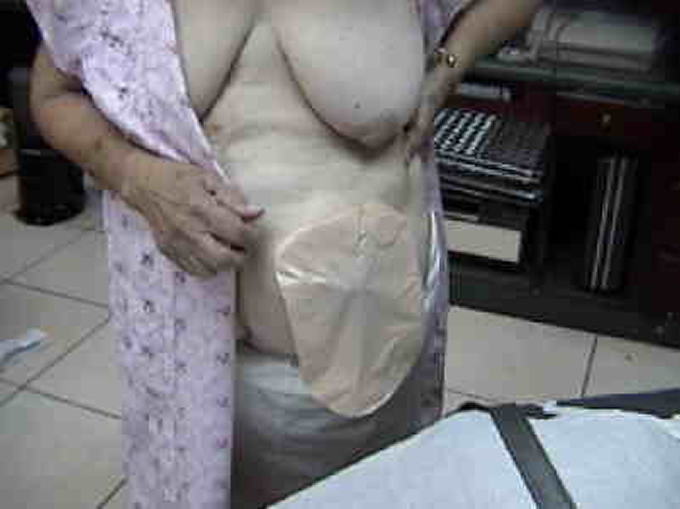
The faeces are collected in a special bag, this uncomfortable situation is for life
since when the colostomy is practiced by cancer in the area of the anus and rectum, sphincters are lost.
So if you are an adult consult a medical expert and Practise full colon study at least every five years as a preventive measure.
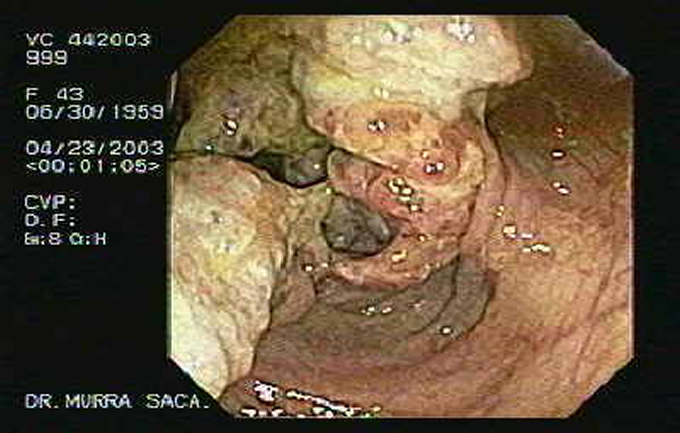
Endoscopic image of cecumcancer. 43 year old-female, who has had
weight loss of 20 pounds and anemia. Click on image to enlarge.

Colonoscopy Video Image where there is a rectal cancer.
Cclick on the image to watch the video.
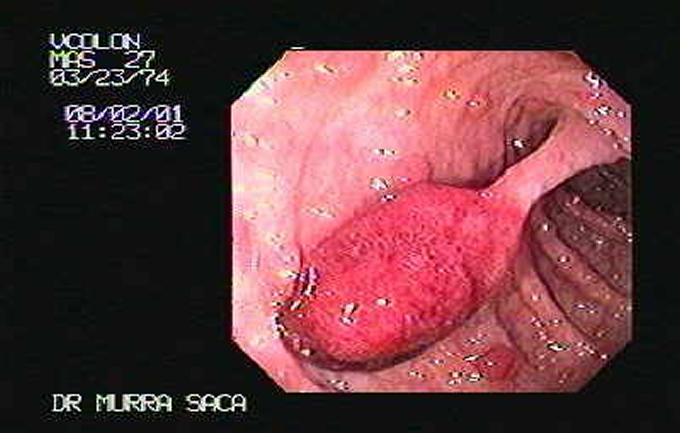
In endoscopic image shows multiple polyps of the colon, usually these colon tumors are asymptomatic spend several years before they become cancer, so they should have this test and remove these small tumors in the same colonoscopy with polypectomy.
Endoscopic Polypectomy of a Rectal Polyp
Endoscopy Polypectomy of Polyp of Descending Colon
Endoscopy: Polypectomy of a Giant Polyp
Endoscopic Polypectomy of Giant Polyp
Endoscopic Resection of Giant Tubulo-Villous Mass of the Descending Colon
Colonoscopy of Juvenile Polyposis
Non Familial Juvenile Polyposis, Polypectomy of Multiple Polyps, First Colonoscopy
Non-Familial Juvenile Polyposis, Polypectomy of Multiple Polyps, Second Colonoscopy
The Endoscopic Symphony No 40 by MurraSaca
See links:
CDC Department of Health and Human Services Center for Disease Control and Prevention
Cáncer de Colon II
Cáncer de Colon III