HOW THE CANCER COMES?
A cancer is an uncontrolled proliferation of cells. In some the rate is fast; in others, slow; but in all cancers the cells never stop dividing. This distinguishes cancers - malign tumors or malignancies - from benign growths like moles where their cells eventually stop dividing.
Cancers are clones. No matter how many trillions of cells are present in the cancer, they are all descended from a single ancestral cell.
Cancers begin as a primary tumor. At some point, however, cells break away from the primary tumor and - traveling in blood and lymph - establish metastases in other locations of the body. Metastasis is what usually kills the patient.
Cancer is a much feared disease that is responsible for millions of deaths worldwide.
Throughout history, the incidence of most types of cancer is steadily on the rise, due to a diversity of factors, such as a changing lifestyle of many human beings, increasing environmental contamination or increasing exposure to ionizing radiation.
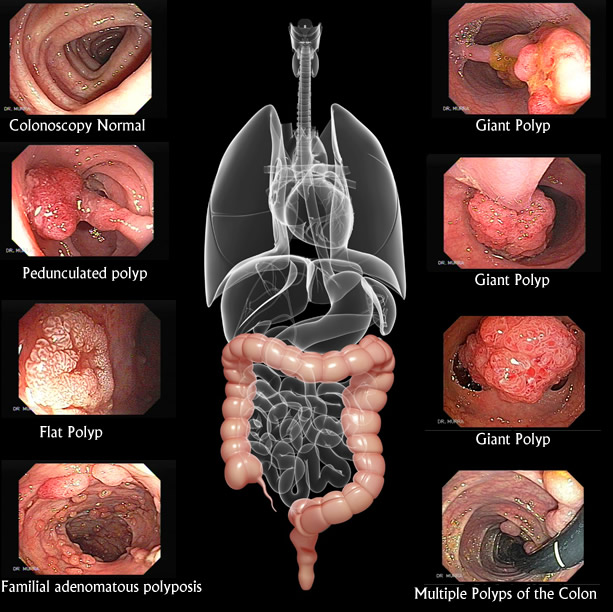
How does a cancer develop? In most cases the evolution of a cancer is a silent development that goes unnoticed. In the G.I. tract a small polyp may grow over many years until it degenerates and becomes cancerous
Recommended Diagnostic Medical Exams for Adults:
Mammography , yearly over the age of forty (asymptomatic women)
Prostate Specific Antigen (PSA Test),
Digital Rectal Examination and Prostate Ultrasound, yearly, in asymptomatic men over fifty.
Upper G.I. tract endoscopy, every 3 years.
Colonoscopy, every four years (every 5 years over the age of fifty)
Pap smear of the Cervix, yearly for asymptomatic women.
Cardiac Stress Test.
It is important to point out that a digital rectal examination is an important part of the clinical examination and any medical check-up is incomplete without it. A rectal exam may discover a rectal carcinoma in its initial stage, before it becomes incurable. An undetected rectal carcinoma will often lead to surgical resection of the rectum and the necessity of a permanenet colostomy, with all the inconveniences that are associated with it.
Defining Cancer
Cancer is a term used for diseases in which abnormal cells divide without control and are able to invade other tissues. Cancer cells can spread to other parts of the body through the blood and lymph systems.
Cancer is not just one disease but many diseases. There are more than 100 different types of cancer. Most cancers are named for the organ or type of cell in which they start - for example, cancer that begins in the colon is called colon cancer; cancer that begins in melanocytes of the skin is called melanoma.
Cancer types can be grouped into broader categories. The main categories of cancer include:
- Carcinoma - cancer that begins in the skin or in tissues that line or cover internal organs. There are a number of subtypes of carcinoma, including adenocarcinoma, basal cell carcinoma, squamous cell carcinoma, and transitional cell carcinoma.
- Sarcoma - cancer that begins in bone, cartilage, fat, muscle, blood vessels, or other connective or supportive tissue.
- Leukemia - cancer that starts in blood-forming tissue such as the bone marrow and causes large numbers of abnormal blood cells to be produced and enter the blood.
- Lymphoma and myeloma - cancers that begin in the cells of the immune system.
- Central nervous system cancers - cancers that begin in the tissues of the brain and spinal cord.
How does cancer begin?
Your body is made up of 100 million million cells. Cancer can start when just one of them begins to grow and multiply too much. The result is a growth called a tumour. Benign tumours are localised growths - they only cause problems if they put pressure on nearby tissues, such as the brain. Much more serious are malignant tumours, which invade the surrounding body tissues. Some malignant tumours also spread throughout the body via the bloodstream: a process called metastasis.
What is cancer recurrence?
Cancer recurrence is defined as the return of cancer after treatment and after a period of time
during which the cancer cannot be detected. (The length of time is not clearly defined.) The same
cancer may come back where it first started or somewhere else in the body. For example, prostate
cancer may return in the area of the prostate gland (even if the gland was removed), or it may
come back in the bones. In either case it’s a prostate cancer recurrence.
The difference between recurrence and progression
When cancer spreads or gets worse it is called progression. Sometimes it’s hard to tell the
difference between recurrence and progression. For example, if the cancer has been gone for only
3 months before it comes back, was it ever really gone? Is this a recurrence or progression?
Chances are this is not really a recurrence. It’s likely 1 of 2 things happen in cases like this: One is
that surgery left behind small clusters of cancer cells that could not be seen or found on scans or
other tests. Over time they grow large enough to be detected or cause symptoms. These cancers
tend to be very aggressive, or fast-growing.
The second possibility is that the cancer may be resistant to treatment. Chemotherapy (chemo) or
radiation may have killed most of the cancer cells, but some of them were either not affected or
changed enough to survive the treatment. Any cancer cells left behind can then grow and show up
again.
The less time between when the cancer was thought to be gone and the time it came back, the more
serious the situation. Most doctors would agree that 3 months of appearing to be cancer-free before
cancer returns is too short to be considered a recurrence. There’s no standard period of time within
the definition of recurrence, but most doctors consider a cancer to be a recurrence if you’ve had no
signs of cancer for at least a year. If your cancer has been gone for only 3 months, this would most
likely be a progression of your disease. In this case, the doctors would assume that the cancer
never went away totally, even though they could not find it with any tests.
What are the types of recurrence?
There are different types of cancer recurrence:
• Local recurrence means that the cancer has come back in the same place it first started.
• Regional recurrence means that the cancer has come back in the lymph nodes near the place it
started.
• Distant recurrence means the cancer has come back in another part of the body, some distance
from where it started (often the lungs, liver, bone marrow, or brain).
If you have a cancer recurrence, your doctor can give you the best information about what type of
recurrence you have and what it means to have that type. You will also want to find out your
options for treatment and outlook (prognosis). See the section, “Treating recurrence.”
What Is Cancer?
The word cancer actually refers to many diseases, not one. In fact, there are more than 100 types of diseases known collectively as cancer. What they all have in common is the overgrowth of cells, tiny units that make up all living things. Cancer (also known as malignancy, pronounced: muh-lig-nun-see) occurs when cells begin to grow and multiply in an uncontrolled way.
Normal body cells grow and divide over a period of time until they eventually die. But cancer cells continue to grow and divide and grow and divide. Eventually, they gather to form tumors. Tumors (pronounced: too-murz) are lumps that can interfere with the body's normal processes. Sometimes cells from a tumor break away and travel to a different tissue or organ. This is called metastasis
What causes cancer?
Cancer is abnormal cell growth, which is the result of damage - mutation - to certain crucial genes, the cell's instructions for making the proteins it needs to survive, grow and multiply. Many factors can affect the chances of the gene damage that may eventually lead to cancer, including cigarette smoke and other chemicals, a poor diet, ultraviolet radiation that causes sunburn, as well as some infections. Chemicals that cause cancer are called carcinogens.
How is cancer detected?
Regular screening already detects some cancers in their early stages - for example smear tests for cervical cancer and mammograms for breast cancer colonoscopy for colorectal cancer.
Can cancer be prevented?
There are many ways in which your risk of cancer can be reduced, either by preventing it or detecting it in its early stages. You can reduce your risk of cancer by not smoking, cutting your alcohol intake, being a healthy weight and eating a balanced diet, taking exercise and protecting yourself from the sun.
What does your immune system do?
Your immune system is your body's defence against infection and illness. It recognises the cells that make up your body, and will try to get rid of anything unfamiliar. It destroys germs (bacteria and viruses) and parasites. But this defence system can also cause problems. It will attack donated organs or blood from another person, unless carefully matched. It may overreact to harmless invaders such as pollen grains, causing hayfever. In some cases (autoimmune diseases), the immune system turns against the body's own cells.
-
 Large villous adenoma.
Large villous adenoma.
precancerous lesion, 40 % of thes villous adenoma. can degenerate in a colonic cancer
Clic here to see the video clip
-

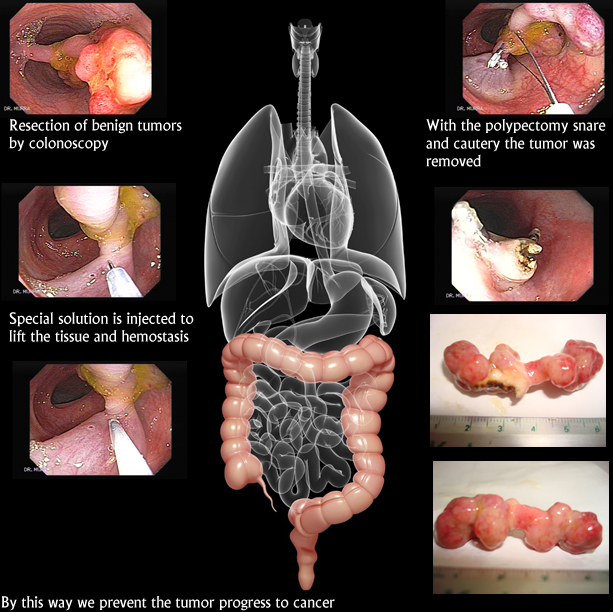
Polypectomy of a rectal polyp, an endoscopic procedure which makes open surgery unnecessary.
Clic here to see thwe video clip
-
 HOW THE CANCER COMES?
HOW THE CANCER COMES?
Images showing the development of a cancer:
-
 HOW THE CANCER COMES?
HOW THE CANCER COMES?
Colon cancer, like all cancers, develops silently and proves to be in an advanced state when clinical symptoms become apparent.
-

Rectal Carcinoma that originates from a rectal polyp
"The theory adenoma carcinoma" Its erly dectection
has become a gold standard for the gastroenterologist.
Clic here to download the video clip.
Polypectomy
The method used to perform colonic polypectomies during colonoscopy depends on the size, shape and histological type of the polyp to be removed. Prior to performing polypectomy, polyps can be biopsied and examined histologically to determine the need to perform polypectomy.
Gastrointestinal polyps can be removed endoscopically through colonoscopy or esophagogastroduodenoscopy, or surgically if the polyp is too large to be removed endoscopically.
The Gastric Cancer Gran Concerto
Endoscopy of Ulcerated Stomach Cancer
Endoscopy of Ulcerated Stomach Cancer in a 34 year-old
Endoscopy of a Gastric Cancer
Stomach Cancer
The Endoscopic Symphony No 40 by MurraSaca
Endoscopic Polypectomy of a Rectal Polyp
Endoscopy Polypectomy of Polyp of Descending Colon
Endoscopy: Polypectomy of a Giant Polyp
Endoscopic Polypectomy of Giant Polyp
Endoscopic Resection of Giant Tubulo-Villous Mass of the Descending Colon
Colonoscopy of Juvenile Polyposis
Non Familial Juvenile Polyposis, Polypectomy of Multiple Polyps, First Colonoscopy
Non-Familial Juvenile Polyposis, Polypectomy of Multiple Polyps, Second Colonoscopy
The Untold History of The Gastrointestinal Endoscopy Part 2 (2/6)
The Untold History of The Gastrointestinal Endoscopy Part 3 (3/6)
The Untold History of The Gastrointestinal Endoscopy Part 4 (4/6)
The Untold History of The Gastrointestinal Endoscopy Part 5 (5/6)
The Untold History of The Gastrointestinal Endoscopy Part 6 (6/6)